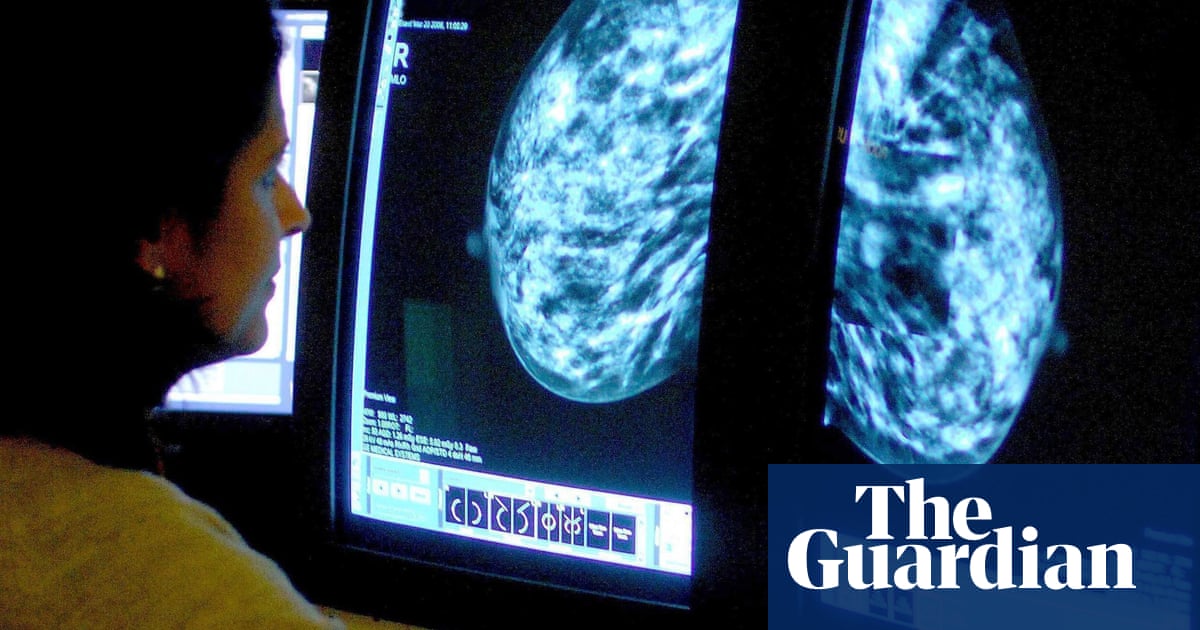
A device relying on artificial intelligence has been developed to pinpoint breast cancer patients at higher risk of encountering adverse effects post-treatment.
Globally, approximately 2 million individuals receive a diagnosis of this ailment annually, making it the most prevalent cancer among women in the majority of regions.
While there has been a rise in success rates in recent years, some patients have faced debilitating side effects following treatment. Nonetheless, enhanced awareness, early detection, and a broader array of treatment choices have bolstered survival rates.
An international coalition of medical professionals, scientists, and researchers has devised an AI tool capable of gauging the likelihood of post-surgical and radiotherapy complications. Currently undergoing trials in the UK, France, and the Netherlands, these systems have the potential to facilitate personalized care for individuals.
Dr. Tim Rattay, a consultant breast surgeon and associate professor at the University of Leicester, expressed, “Fortunately, long-term survival rates for breast cancer continue to improve, but for some patients, this progress entails coping with treatment side effects.” These effects may encompass skin alterations, scarring, lymphoedema (painful arm swelling), and even cardiac issues resulting from radiation therapy.
“We are in the process of developing an AI tool to apprise doctors and patients about the risk of enduring chronic arm swelling post breast cancer surgery and radiotherapy. Our aim is for this tool to assist in selecting radiation treatment options, thereby minimizing side effects for all patients,” Dr. Rattay explained.
Drawing insights from a cohort of 6,361 breast cancer patients, the AI tool was trained to forecast lymphoedema occurrence up to three years post-surgery and radiotherapy. Patients flagged as predisposed to arm swelling could potentially receive alternative treatments or additional care pre- and post-treatment.
The finalized, most effective model integrates 32 distinct patient and treatment attributes, such as chemotherapy administration, sentinel lymph node biopsy under the armpit, and the type of radiotherapy employed, as outlined by Dr. Guido Bologna, associate professor at the University of Applied Sciences and Arts of Western Switzerland in Geneva.
With an 81.6% accuracy rate in predicting lymphoedema and a 73.4% overall predictive precision, the AI tool proves valuable in identifying patients at risk. Dr. Rattay suggested that patients at elevated risk of arm swelling could benefit from supplementary measures like wearing an arm compression sleeve during treatment, known to mitigate long-term arm swelling. This information can also guide physicians in deliberating lymph node irradiation options for patients where the benefits may be somewhat limited.
Presenting at the European Breast Cancer Conference in Milan, Dr. Rattay emphasized that the technology constituted an “explainable AI tool,” providing rationale for its decisions.
“This not only simplifies decision-making for doctors but also enables them to furnish evidence-based justifications to their patients,” he added.
The ongoing Pre-Act project, a two-year clinical trial, will be overseen by the research team, aiming to enroll 780 patients. Additionally, efforts are underway to devise a tool for predicting other side effects like heart and skin damage.
Dr. Simon Vincent, director of research, support, and influencing at Breast Cancer Now, stressed the urgency of enhancing treatments. He remarked, “This groundbreaking initiative seeks to explore whether AI can facilitate personalized care for breast cancer patients, reducing side effects such as chronic arm swelling post-surgery and radiotherapy.
Awaiting the trial results, as the project is still in its nascent stages and necessitates further evidence before contemplating the integration of the AI tool into medical environments.
In a separate development, Italian researchers found that utilizing combined positron emission tomography and magnetic resonance imaging (PET-MRI) scans enabled doctors to detect the spread of a breast cancer patient’s tumor, leading to alternative therapy options like chemotherapy or different surgical approaches.
Concurrently, researchers from the Netherlands revealed that young breast cancer patients who received a low-dose radiotherapy boost at the site of tumor removal, alongside whole breast radiotherapy, remained free of local recurrence even after ten years.